 Have you heard of the “Baader-Meinhof” effect? If not, I’m positive you’ll soon be seeing evidence of it everywhere.
Have you heard of the “Baader-Meinhof” effect? If not, I’m positive you’ll soon be seeing evidence of it everywhere.
That’s what “it” is, by the way — that curious experience of seeing something you’ve just noticed, been told of, or thought about, cropping up all around you. So …
You buy a car and suddenly it’s everywhere. That outfit you thought was so unique? Boom! Everyone is sporting it. How about the conversation you just had with your friend? You know, the one that was so stimulating and interesting? Now the subject is on everyone’s lips.
Depending on your level of self-esteem or degree of narcissism, Baader-Meinhof either leaves you feeling on the “cutting edge” of cultural trends or constantly lagging behind others. For me, it’s generally the latter. And recently, its a feeling that has been dogging me a fair bit.
The subject? Trauma.
Whether simple or complex, ongoing or one-off, experienced as a child or adult, trauma is the topic de jour — a cause célèbre linked to an ever-growing list of problems, including depression, anxiety, dissociation, insomnia, headaches, stomachaches, asthma, stroke, diabetes, and most recently, ADHD.
ever-growing list of problems, including depression, anxiety, dissociation, insomnia, headaches, stomachaches, asthma, stroke, diabetes, and most recently, ADHD.
Then, of course, there are the offers for training. Is it just me or is trauma the subject of every other email solicitation, podcast announcement, and printed flyer?
The truth is our field has been here many times before. Over the last 25 years, depression, multiple personality disorder, rapid cycling bipolar disorder II, attention deficit disorder, and borderline personality disorder have all burst on the scene, enjoyed a period of intense professional interest, and then receded into the background.
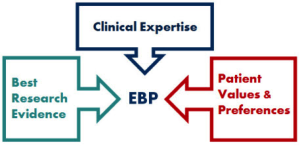
Available evidence makes clear this pattern — aha, whoa, and hmm what’s next? — is far from benign. While identifying who is suffering and why is an important and noble endeavor, outcomes of mental healthcare have not improved over the last 40 years. What’s more, no evidence exists that training in treatment modalities specific to any particular diagnosis — the popularly-termed, “evidence-based” practices — improves effectiveness. Problematically, studies do show undergoing such training increases practitioner perception of enhanced competence (Neimeyer, Taylor, & Cox, 2012) .
 On more than one occasion, I’ve witnessed advocates of particular treatment methods claim it’s unethical for a therapist to work with people who’ve experienced a trauma if they haven’t been trained in a specific “trauma-focused” approach. It’s a curious statement — one which, given the evidence, can only be meant to bully and shame practitioners into going along with the crowd. Data on the subject are clear and date back over a decade (1, 2, 3). In case of any doubt, a brand new review of the research, published in the journal Psychotherapy, concludes, “There are no clinically meaningful differences between … treatment methods for trauma … [including those] designed intentionally to omit components [believed essential to] effective treatments (viz., exposure, cognitive restructuring, and focus on trauma)” (p. 393).
On more than one occasion, I’ve witnessed advocates of particular treatment methods claim it’s unethical for a therapist to work with people who’ve experienced a trauma if they haven’t been trained in a specific “trauma-focused” approach. It’s a curious statement — one which, given the evidence, can only be meant to bully and shame practitioners into going along with the crowd. Data on the subject are clear and date back over a decade (1, 2, 3). In case of any doubt, a brand new review of the research, published in the journal Psychotherapy, concludes, “There are no clinically meaningful differences between … treatment methods for trauma … [including those] designed intentionally to omit components [believed essential to] effective treatments (viz., exposure, cognitive restructuring, and focus on trauma)” (p. 393).
If you find the results reported in the preceding paragraph confusing or unbelievable, recalling the “Baader-Meinhof” effect can be help. It reminds us that despite its current popularity in professional discourse, trauma and its treatment is nothing new. Truth is, therapists have always been helping those who’ve suffered its effects. More, while the field’s outcomes have not improved over time, studies of real world practitioners show they generally achieve results on par with those obtained in studies of so-called evidence-based treatments 1, 2, 3).
Of course, none of the foregoing means nothing can be done to improve our effectiveness. As my Swedish grandmother Stena used to say, “The room for improvement is the biggest one in our house!” 
To get started, or fine tune your professional development efforts, listen in to an interview I did recently with Elizabeth Irias from Clearly Clinical (an approved provider of CEU’s for APA, NBCC, NAADAC, CCAPP, and CAMFT). Available here: What Every Therapist Needs To Know: Lessons From The Research, Ep. 61.
In it, I lay out several, concrete, evidence-based steps, practitioners can take to improve their therapeutic effectiveness. It’s FREE, plus you can earn a FREE hour of CE credit. Additionally, if follow them on Instagram and leave a comment on this post, you’ll be automatically entered into a contest for one year of free, unlimited continuing education — the winner to be announced on October 31st, 2019.
Until next time,
Scott
Scott D. Miller, Ph.D.
Director, International Center for Clinical Excellence


–




















































































.png)
.jpg)




.jpg)


.jpg)

.jpg)
.jpg)




